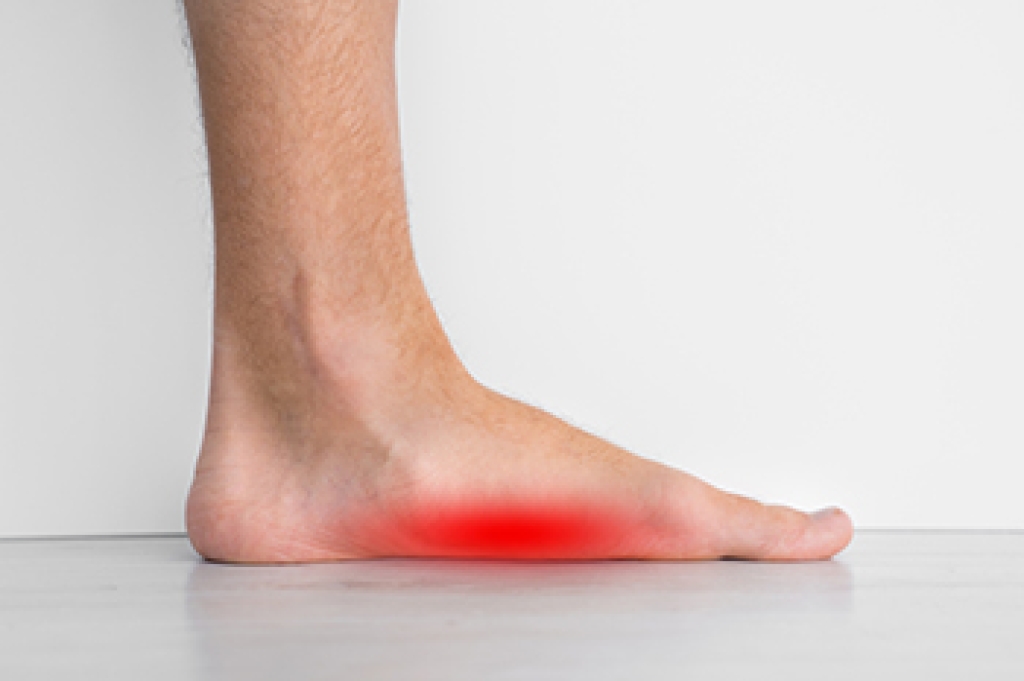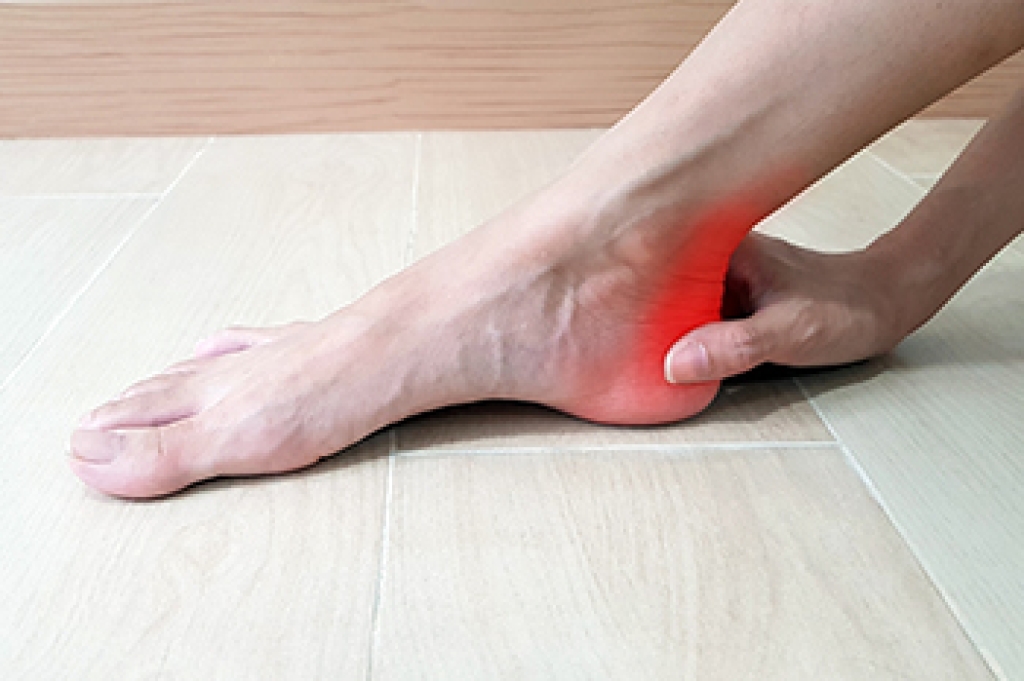
Achilles tendon heel pain, medically known as Achilles tendon enthesopathy, occurs where the Achilles tendon attaches to the back of the heel bone. Patients with this condition often feel pain at the back of the heel, especially during walking or ankle movement. The condition is caused by repetitive strain on the Achilles tendon, which can result from a sedentary lifestyle, being overweight, or overuse from athletic activities. Risk factors may also include age, certain medications, or underlying arthritis. Diagnosis typically involves a podiatrist performing a physical examination to check for tenderness and flexibility of the ankle. Effective treatments include reducing strain on the tendon, such as using heel lifts, creating a personalized stretching regimen, and addressing any biomechanical issues. A podiatrist may also recommend supportive footwear or other therapeutic techniques to improve healing and alleviate discomfort. If you have heel pain caused by an Achilles tendon injury it is suggested that you schedule an appointment with a podiatrist for treatment.
Achilles tendon injuries need immediate attention to avoid future complications. If you have any concerns, contact Mark Isenberg, DPM of Center for Podiatric Excellence. Our doctor can provide the care you need to keep you pain-free and on your feet.
What Is the Achilles Tendon?
The Achilles tendon is a tendon that connects the lower leg muscles and calf to the heel of the foot. It is the strongest tendon in the human body and is essential for making movement possible. Because this tendon is such an integral part of the body, any injuries to it can create immense difficulties and should immediately be presented to a doctor.
What Are the Symptoms of an Achilles Tendon Injury?
There are various types of injuries that can affect the Achilles tendon. The two most common injuries are Achilles tendinitis and ruptures of the tendon.
Achilles Tendinitis Symptoms
- Inflammation
- Dull to severe pain
- Increased blood flow to the tendon
- Thickening of the tendon
Rupture Symptoms
- Extreme pain and swelling in the foot
- Total immobility
Treatment and Prevention
Achilles tendon injuries are diagnosed by a thorough physical evaluation, which can include an MRI. Treatment involves rest, physical therapy, and in some cases, surgery. However, various preventative measures can be taken to avoid these injuries, such as:
- Thorough stretching of the tendon before and after exercise
- Strengthening exercises like calf raises, squats, leg curls, leg extensions, leg raises, lunges, and leg presses
If you have any questions please feel free to contact our office located in Pensacola, FL . We offer the newest diagnostic tools and technology to treat your foot and ankle needs.